OVERVIEW:
Physician burnout is an epidemic threatening our healthcare system, as the pressures and burdens on physicians increase due to technological and societal changes.
Penn Medicine has an ongoing inquiry, seeking ways to alleviate physician burnout and in 2017 partnered with the Integrated Product Design program to explore ways to prevent burnout and change the role of wellness in doctor culture.
This 9 week research project culminated in a roadmap of initiatives that lead to the “Doctor of the Future” and a communication strategy to support the Innovation Team as they moved toward this goal.
SKILLS: Product Management, Design Strategy, Research, Roadmapping
COLLABORATORS: James Sannino, Mike Lytle

Physician burnout
A recent Mayo Clinic study reports that over 54% of physicians have at least one symptom of burnout, with an over 10% increase between 2011 and 2014. The rigorous standards and high-intensity environment at Penn Medicine's Hospitals and clinics put doctors at serious risk for burnout.
The 3 primary symptoms of Physician Burnout are emotional exhaustion, depersonalization, reduced confidence in skills. Research points to work-life imbalance, too little time with patients and a physician’s lack of control over their work life as the key factors leading to burnout.
How can a health system as complex as Penn Medicine help physicians combat the real effects of physician burnout? And what are the nuances of this condition for faculty physicians who carry the even greater weight of their teaching responsibilities? Our team set out to understand the daily workflow and challenges faced by Penn Faculty in the context of the hospital system in order to help Penn Medicine understand how it can provide faculty with wellness opportunities in their daily work lives.
Process
To address the increasing rate of burnout we needed to understand what factors were causing stress in the lives of Penn Med faculty.
Process Artifacts:
Card sort development






Framework
We applied Maslow’s Hierarchy as a framework to understand doctors’ needs and found that in the hospital setting the hierarchy is turned on its head.
Insights
Maslow's theory suggests that the most basic level of needs must be met before an individual will strongly desire (or focus motivation upon) the secondary or higher level needs. Yet in the hospital setting the hierarchy is turned on its head, with higher level needs playing a more central role for physicians, while they are asked to ignore lower needs, for example: not eat or use the restroom for up to 10 hours while in surgery. Needs like self actualization are more clearly met, as doctors are empowered to be who they are meant to be in their work-life.



Analysis
Diverse faculty have diverse needs:
Designing a solution for physician burnout is complex as diverse faculty have diverse needs. Influencing factors:
● Stage in career/seniority
● Gender and family
● Generational values
● Daily experience/duties vary across medicine, surgery, research, teaching & administration
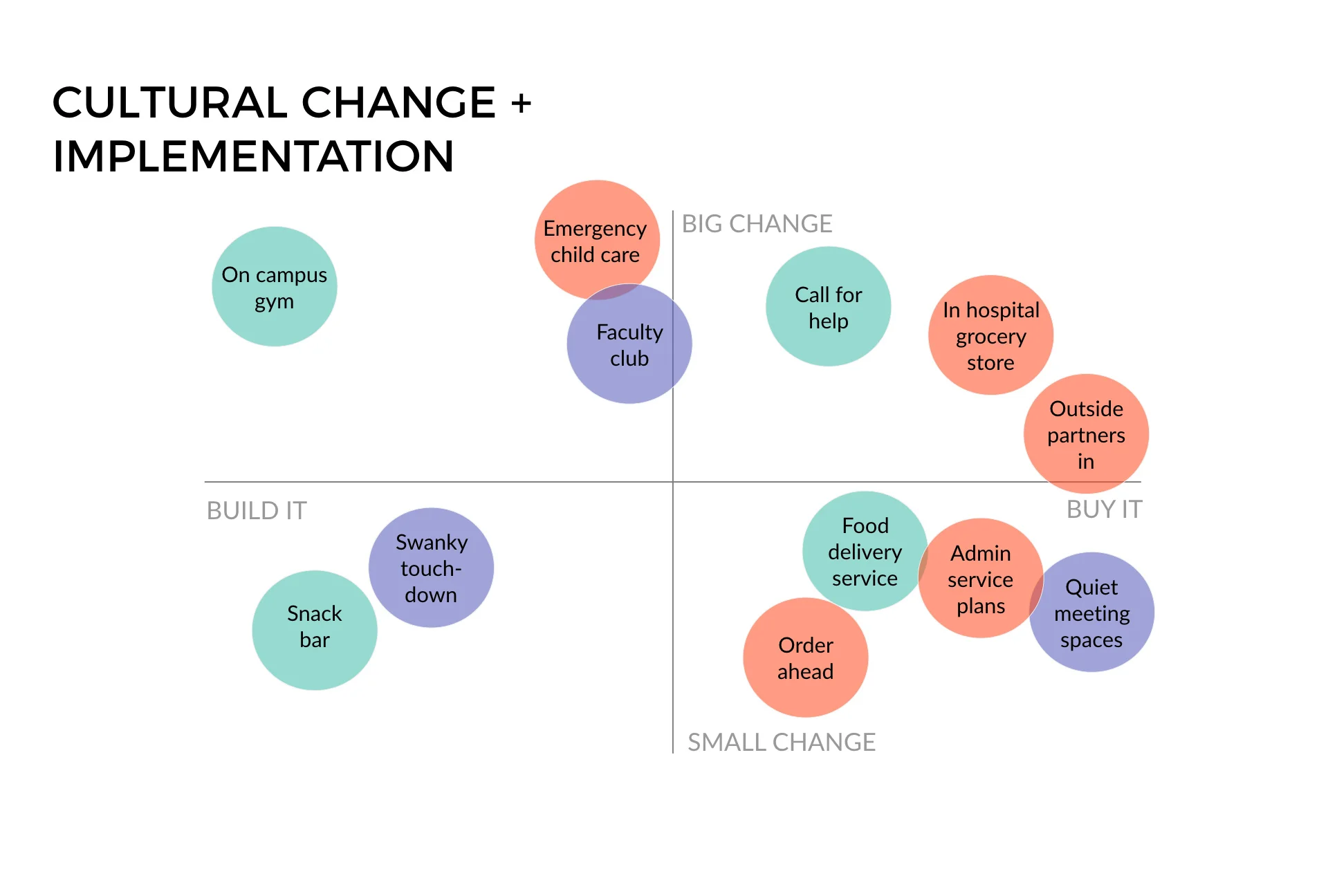
These solutions can be implemented on a range of scales across the hospital ecosystem: the individual, the network of connected staff, and solutions in the hospital environment.
Team ideation resulted in a deck of opportunities, which we tested with our interviewees. Integrating the interviewee feedback, we ranked our opportunities.
Deliverables
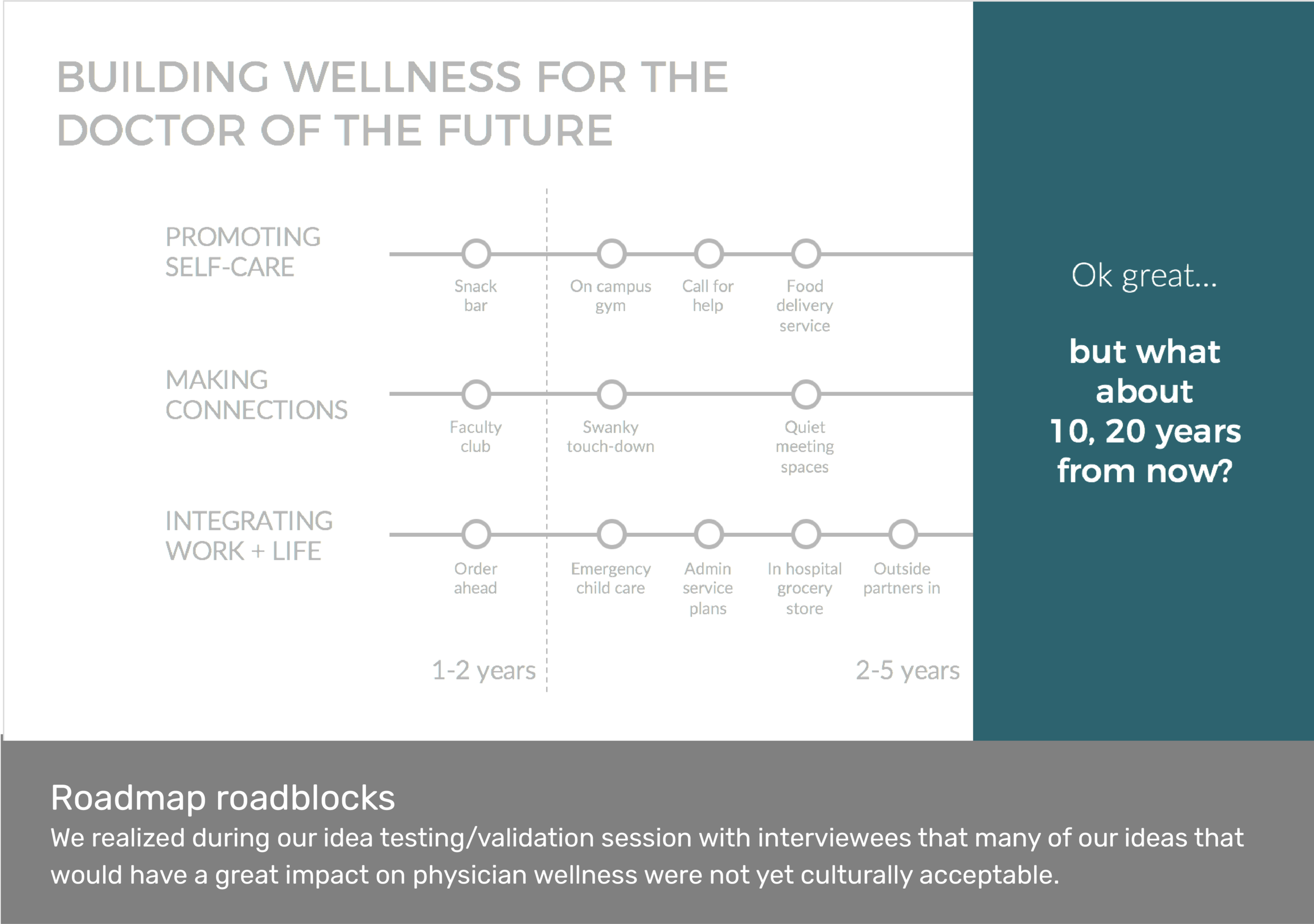
Roadmap
We grouped our chosen ideas by insight and strategically mapped them on a timeline to provide Penn Medicine with a roadmap to better physician wellbeing.
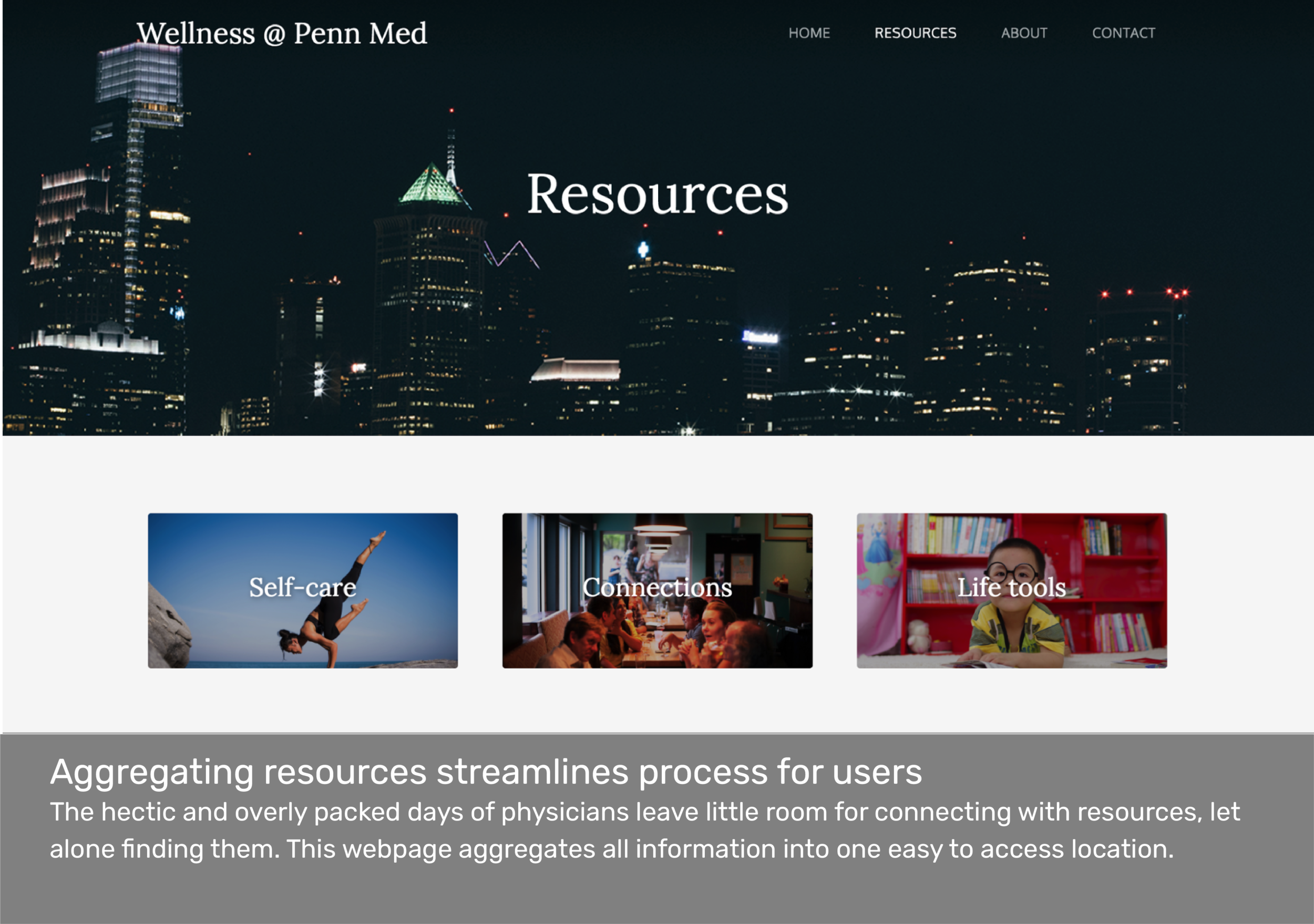
Communication Strategy
During our research we discovered a handful of resources for physician wellness that the majority of our interviewees were not aware of. Not only must Penn Medicine implement initiatives to solve for physician burnout, but these solutions must be communicated to lead busy and over-stressed practitioners to the resources they need.
Doctors are inundated with information. The hospital must be clear that it values well-being using multi-channel communication and cultural initiatives.